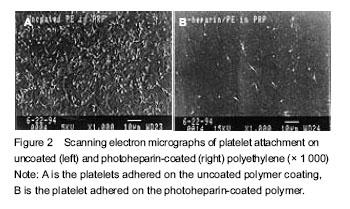
| [1] Boretos JW, Eden M, Contemporary Biomaterials: Material and Host Response, Clinical Applications, New Technology, and Legal Aspects. Park Ridge, NJ: Noyes Publications. 1984:232-233.
[2] March J. Advanced Organic Chemistry, Reactions, Mechanisms and Structure. 3rd ed. New York: John Wiley & Sons inc. 1985:216.
[3] Wang DA, Chen BL, Ji J, et al. Selective adsorption of serum albumin on biomedical polyurethanes modified by a poly(ethylene oxide) coupling-polymer with cibacron blue (F3G-A) endgroups. Bioconjug Chem. 2002;13(4): 792-803.
[4] Anderson AB, Tran TH, Hamilton MJ, et al. Platelet deposition and fibrinogen binding on surfaces coated with heparin or friction-reducing polymers. AJNR Am J Neuroradiol. 1996;17(5):859-863.
[5] Chen BL, Wang DA. Phase II study on surface construction and biocompatibility of polymer materials as cardiovascular devices: surface construction and biological responses. Zhongguo Zuzhi Gongcheng Yanjiu. 2014;18(21): 3412-3419.
[6] Chen BL, Wang DA. Surface construction and biocompatibility of polymeric used for cardiovascular medical device. Zhongguo Zuzhi Gongcheng Yanjiu. 2013;17(34):6183-6192.
[7] Chen BL, Wang DA. Hemocompatibility of biomedical polymeric materials: design of anticoagulant materials. Zhongguo Zuzhi Gongcheng Yanjiu. 2012;16(34): 6393-6396.
[8] Chen BL, Wang DA. Preparation and mechanism of anticoagulatent biomedical polymer materials with blood compatibility. Biocompatibility of a magnesium-zinc alloy implanted in rat cecum. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2011;15(29):5507-5510.
[9] Chen BL, Wang DA, Feng LX. Investigation on methods of surface modification of tissue engineering materials: polymer surface group transformation and bioactive molecule immobilization. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2010;14(3):552-554.
[10] Chen BL, Wang DA, Feng LX. Surface modification of tissue-engineered materials plasma and grafting modification. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2009;13(3):587-590.
[11] Chen BL, Wang DA, Feng LX. Application of polymer biomaterials in the tissue engineering. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2008;12(6): 1189-1192.
[12] Chen BL, Wang DA, Feng LX. Polymer porous membrane prepared using thermally induced phase separation. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2007;11(40):8217-8219.
[13] Chen BL, Wang DA, Feng LX. Topology of tissue engineering material surface for cell compatibility. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2007;11(18):3653-3656.
[14] Chen BL, Wang DA, Feng LX. Effects of physical and chemical properties of tissue engineered material surface on cell compatibility. Zhongguo Zuzhi Gongcheng Yanjiu yu Linchuang Kangfu. 2007;11(1):197-200.
[15] Chen BL, Wang DA, Feng LX. Cytological effect of tissue engineering materials with cell compatibility. Zhongguo Lincuang Kangfu. 2006;10(45):225-227.
[16] Chen BL, Wang DA, Feng LX, et al. The application of biomedical tissue engineering and the polymer tissue engineering material. Gaoshi Like Xuekan. 2007;27(1): 24-26.
[17] Chen BL, Wang DA, Feng LX, et al. Study on the blood compatibility of biomedical ploymer materials--project of antithromboeicity materials. Suihua Xueyuan Xuebao. 2007;27(1):186-188.
[18] Chen BL, Wang DA, Feng LX. Study on surfaces modify of the tissue engineering materials and application in the tissue engineering. Hulunbeier Xueyuan Xuebao. 2007; 15(1):52-54.
[19] Chen BL, Wang DA, Feng LX. Study on the tissue compatibility of biomedical ploymer materials--project of tissue-compatibility materials. Hulunbeier Xueyuan Xuebao. 2006;14(6):34-36.
[20] March J. Advanced Organic Chemistry, Reactions, Mechanisms and Structure. 3rd ed. New York: John Wiley & Sons Inc. 1985:1078.
[21] Brown EJ. Complement receptors, adhesion, and phagocytosis. Infect Agents Dis. 1992;1(2):63-70.
[22] Abele JE. Technical considerations: physical properties of balloon catheters, inflation devices and pressure measurement devices. In: Castaned-Zuniga WR, ed. Transluminal Angioplasty. New York: Thieme-Stratton, 1983:20-27.
[23] Triolo PM, Andrade JD. Surface modification and evaluation of some commonly used catheter materials. I. Surface properties. J Biomed Mater Res. 1983;17(1):129-147.
[24] Triolo PM, Andrade JD. Surface modification and characterization of some commonly used catheter materials. II. Friction characterization. J Biomed Mater Res. 1983;17(1):149-165.
[25] Salzman EW, Merill EW. Interaction of blood with artificial surfaces. In: Hemostasis and Thrombosis. 2nd ed. Philadelphia, PA, USA: J.B. Lippincott. 1987:1335-1347.
[26] Chenoweth DE. Complement activation in extracorporeal circuits. Ann N Y Acad Sci. 1987;516:306-313.
[27] Harrison JA, Colton RJ, White CT, et al. Atomistic simulation of the nanoindentation of diamond and graphite surfaces. Materials Research Sjociety, Symp. Proceeding. 1992;239:573.
[28] Hubbell JA, Massia SP, Desai NP, et al. Endothelial cell-selective materials for tissue engineering in the vascular graft via a new receptor. Biotechnology (N Y). 1991;9(6):568-572.
[29] Remes A, Williams DF. Immune response in biocompatibility. Biomaterials. 1992;13(11):731-743.
[30] Esmon CT. Thrombomodulin as a model of molecular mechanisms that modulate protease specificity and function at the vessel surface. FASEB J. 1995;9(10): 946-955.
[31] Plow EF, Herren T, Redlitz A, et al. The cell biology of the plasminogen system. FASEB J. 1995;9(10):939-945.
[32] Hårdhammar PA, van Beusekom HM, Emanuelsson HU, et al. Reduction in thrombotic events with heparin-coated Palmaz-Schatz stents in normal porcine coronary arteries. Circulation. 1996;93(3):423-430.
[33] Pasic M, Müller-Glauser W, von Segesser LK, et al. Superior late patency of small-diameter Dacron grafts seeded with omental microvascular cells: an experimental study. Ann Thorac Surg. 1994;58(3):677-684.
[34] Greisler HP, Klosak J, Dennis JW, et al. Endothelial cell growth factor attachment to biomaterials. ASAIO Trans. 1986;32(1):346-349.
[35] Gray JL, Kang SS, Zenni GC, et al. FGF-1 affixation stimulates ePTFE endothelialization without intimal hyperplasia. J Surg Res. 1994;57(5):596-612.
[36] Reilly CF, Kindy MS, Brown KE, et al. Heparin prevents vascular smooth muscle cell progression through the G1 phase of the cell cycle. J Biol Chem. 1989;264(12): 6990-6995.
[37] Au YP, Kenagy RD, Clowes MM, et al. Mechanisms of inhibition by heparin of vascular smooth muscle cell proliferation and migration. Haemostasis. 1993;23 Suppl 1:177-182.
[38] Kang SS, Gosselin C, Ren D, et al. Selective stimulation of endothelial cell proliferation with inhibition of smooth muscle cell proliferation by fibroblast growth factor-1 plus heparin delivered from fibrin glue suspensions. Surgery. 1995;118(2):280-287.
[39] Gosselin C, Ren D, Ellinger J, et al. In vivo platelet deposition on polytetrafluoroethylene coated with fibrin glue containing fibroblast growth factor 1 and heparin in a canine model. Am J Surg. 1995;170(2):126-130.
[40] Greisler HP, Ellinger J, Schwarcz TH, et al. Arterial regeneration over polydioxanone prostheses in the rabbit. Arch Surg. 1987;122(6):715-721.
[41] Greisler HP, Schwarcz TH, Ellinger J, et al. Dacron inhibition of arterial regenerative activities. J Vasc Surg. 1986;3(5):747-756.
[42] Greisler HP, Dennis JW, Endean ED, et al. Derivation of neointima in vascular grafts. Circulation. 1988;78(3 Pt 2):I6-12.
[43] Serruys PW, Emanuelsson H, van der Giessen W, et al. Heparin-coated Palmaz-Schatz stents in human coronary arteries. Early outcome of the Benestent-II Pilot Study. Circulation. 1996;93(3):412-422.
[44] Anderson AB, Enrico LS, Melchior MJ, et al., Photochemical immobilization of heparin to reduce thrombogenesis. Trans Soc Biomat. 1994;17(1):75.
[45] Clapper DL, Hagen KM, Hupfer JM, et al. Covalently immobilized ECM proteins improve patency and endothelialization of 4 mm grafts implanted in dogs. Trans Soc Biomat. 1993;16(1):42.
[46] Sauvage LR, Berger KE, Wood SJ, et al. Interspecies healing of porous arterial prostheses: observations, 1960 to 1974. Arch Surg. 1974;109(5):698-705.
[47] Williams SK, Schneider T, Kapelan B, et al. Formation of a functional endothelium on vascular grafts. J Electron Microsc Tech. 1991;19(4):439-451.
[48] Tweeden KS, Blevitt J, Harasaki H, et al. RGD Modification of Cardiovascular Prosthetic Materials, in Proceedings of the Cardiovascular Science and Technology Conference, Arlington, VA, Association for the Advancement of Medical Instrumentation. 1993;12:124.
[49] Campbell EJ, Chronos NA, Robinson KA, et al. Non-thrombogenic phosphorylcholine coatings stainless steel. Trans Soc Biomat. 1995;18(1):15.
[50] Chronos NA, Robinson KA, Kelly AB, et al. Thromboresistant phosphorylcholine coating for coronary stents. Circulation. 1995;92(suppl I):685.
[51] Ishihara K, Aragaki R, Ueda T, et al. Reduced thrombogenicity of polymers having phospholipid polar groups. J Biomed Mater Res. 1990;24(8):1069-1077.
[52] Eberhart RC, Munro MS, Frautschi JR, et al. Influence of endogenous albumin binding on blood-material interactions. Ann N Y Acad Sci. 1987;516:78-95.
[53] Grasel TG, Pierce JA, Cooper SL. Effects of alkyl grafting on surface properties and blood compatibility of polyurethane block copolymers. J Biomed Mater Res. 1987;21(7):815-842. |